by Brett Bralley | Apr 18, 2022 | Research and Innovation
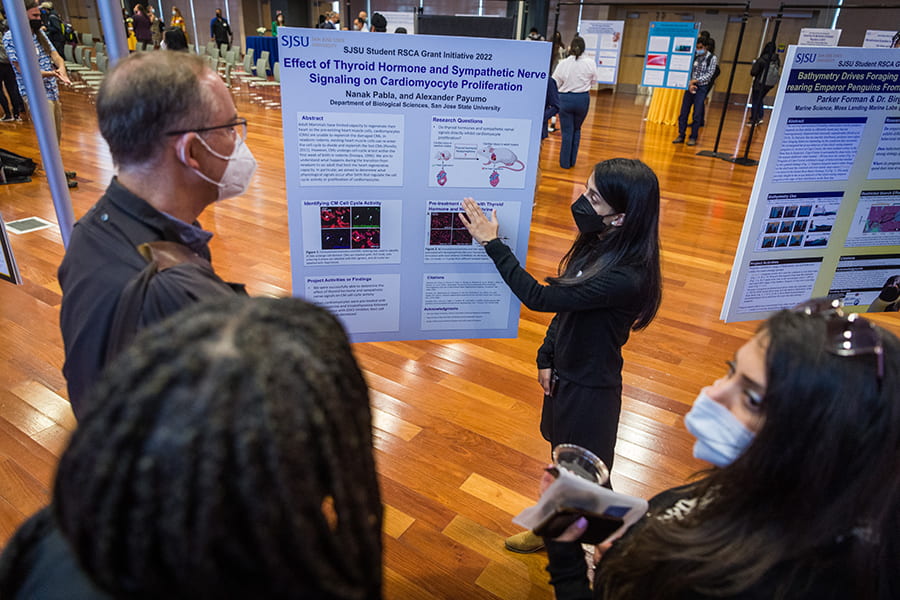
Celebration of Research Event Salutes Faculty and Student Success A researcher shares her work at the annual Celebration of Research, held in-person for the first time in two years. Photo: Robert C. Bain From digital art installations to wildfire tornadoes to...

by Brett Bralley | Mar 15, 2022 | Awards and Achievements
Wildfire Research, Community Clinic Included in $1.5 Trillion Federal Spending Plan Scientists with SJSU’s Wildfire Interdisciplinary Research Center (WIRC) at Milford, California, in summer 2021 observing the Dixie Fire. Photo credit: WIRC Two major San José...

by Brett Bralley | Mar 8, 2022 | Diversity, Equity and Inclusion
Women in Engineering Conference Focuses on ‘Leaders for Tomorrow’ Graphic: SJSU College of Engineering On March 19, about 550 women engineering students will congregate virtually for the eighth annual Silicon Valley Women in Engineering conference, hosted by San José...





